Hope for Stomach Cancer recently spoke with Greg Myers, a gastric cancer diagnosis survivor. There is a common saying that when a person develops cancer, their entire family gets it because of the all-encompassing way that this disease impacts lives. In Greg’s case, as a carrier of the rare CDH1 gene, this was literally the truth. This is his story of battling cancer as a family and finding hope along the way.
Q: Greg, thanks for your willingness to share your story today about your gastric cancer diagnosis. Can you please tell us a little bit about you and your family, along with the story of how you learned about having cancer?
 A: Yes, my name is Greg, and my wife Kristie and I live in California City, CA. I’ve worked for the U.S. Air Force since 1998, and my wife works for the defense company Northrop Grumman. We have two grown children, Kori (28) and Tyler (26).
A: Yes, my name is Greg, and my wife Kristie and I live in California City, CA. I’ve worked for the U.S. Air Force since 1998, and my wife works for the defense company Northrop Grumman. We have two grown children, Kori (28) and Tyler (26).
In early 2021, I began having stomach and digestive problems. I was in the emergency room at one point with a possible blockage, and I started seeing a physician to get insight into what was happening. I was told that I had an intestinal infection and that I’d need to go on a liquid-only diet for 10 days.
As I transitioned off of that diet, I struggled with swallowing solid food. The issue may have existed before the liquid-only diet, but it was clear that something had changed as I tried to consume solid foods again. I spoke with my doctor about my discomfort. I figured it would be a routine case of acid reflux, but my doctor ordered an endoscopy just to be safe.
The endoscopy occurred on June 10th. Shockingly, we learned that there was a 3-centimeter mass in the GE junction between my esophagus and stomach. The doctor rapidly ordered a biopsy, which also took place in June 2021.
I recall being concerned, but life moved forward during this uncertain period. Kristie and I traveled to Hawaii for a fun vacation and went to work as usual.
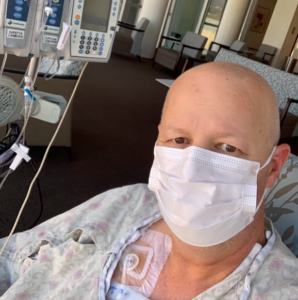 In early July, I received an incoming phone call from the doctor – my biopsy results were ready. Kristie wasn’t home quite yet, but I had the phone on speaker. She walked in the door just as the doctor revealed my gastric cancer diagnosis. I recall her breaking down on the spot as we heard the news.
In early July, I received an incoming phone call from the doctor – my biopsy results were ready. Kristie wasn’t home quite yet, but I had the phone on speaker. She walked in the door just as the doctor revealed my gastric cancer diagnosis. I recall her breaking down on the spot as we heard the news.
After the Gastric cancer diagnosis
Immediately after my diagnosis, I was referred to the City of Hope campus in Lancaster, CA. At this point, I was dealing with the news by avoiding the details. I did not want to know my stage, my prognosis, or my long-term outlook. Kristie, on the other hand, delved into research. Understanding all the ins and outs of stomach cancer was essential for helping her cope.
I met with my oncologist at City of Hope. I was told that I’d need to have four rounds of FLOT treatments, surgery to remove the mass, and then four FLOT treatments after that. I received my port, and in early September I went in for my first FLOT session. Further, I met my surgeon around this time so that we could start planning for the mass removal.
FLOT Treatments
I knew that FLOT treatments were bound to cause some odd side effects. After all, the process introduces some heavy-duty chemicals to your body. My nurses warned me that I needed to be cautious when handling cold items or drinking cold beverages. In fact, they even suggested that I wear gloves when retrieving things from the refrigerator.
After my first FLOT treatment, I recall reaching into the fridge to grab something. I wasn’t wearing gloves since frankly, I wasn’t too concerned about the side effects at that point. It turned out that touching cold items was excruciatingly painful! I dropped what I was holding. Moving forward, this side effect persisted and was especially intense after each FLOT treatment.
In addition to cold sensitivity, I had to change my routines around the house. Kristie and I couldn’t sleep in the same bed or wash our clothing together because the body leeches heavy metals following FLOT treatments.
The CDH1 Study
Despite these setbacks, I managed my early FLOT rounds quite well. During one of these treatments, I spoke with a nurse who invited me to take part in a study that could help me as well as other people battling stomach cancer. The study involved the CDH1 gene, a genetic marker that, if mutated, can greatly increase a person’s chances of having certain cancers.
I agreed to participate in the study. The nurse drew my blood and sent it to the company Invitae for testing.
Around the same time, my doctor ordered a second endoscopy along with an ultrasound to get more clarity on my gastric cancer diagnosis. We needed to determine which stage the cancer was in and see if anything had changed since the last endoscopy.
Admittedly, I was prepared for bad news – so you can imagine my surprise when I learned that my cancer was at stage 2A. This meant that it was in the stomach lining, but had not traveled to other parts of my body. We were elated!
 The CDH1 Mutation: A Complication That No One Expected
The CDH1 Mutation: A Complication That No One Expected
However, there was another challenge to face. My results from the Invitae study were back, and I was positive for a mutation on the CDH1 gene. Mutations are associated with a high risk of hereditary diffuse gastric cancer (HDGC). In fact, up to 70 percent of people with this mutation develop stomach cancer in their lifetimes. Further, since there is a genetic component, everyone in your family is at risk of having the mutation as well. And stomach cancer tends to start earlier for the next generation, too.
I was 49 at the time of my diagnosis. Upon hearing the news about the CDH1 mutation, my thoughts immediately went to my family, including my kids.
Q: Wow, it must have been shocking to receive that news – especially knowing that the gene mutation could affect other people you love. How did your treatment progress, and what happened next with your family?
A: We had already been busy with treatments and procedures before learning this news. However, everything kicked into overdrive after this. I was told that I needed to meet my surgeon right away for genetic counseling. Further, although I was stage 2A, I learned that I would definitely have to have a total gastrectomy as a result of this mutation.
Honestly, I didn’t even realize it was possible to live without a stomach! I was trying to wrap my head around this new reality while determining how to share the news with my kids.
The Next Steps
Several important developments happened at the same time. First, I was referred to an excellent surgeon named Dr. Yanghee Woo at the City of Hope campus in Duarte. This highly-specialized surgeon would be the one responsible for my total gastrectomy.
Next, I was going through genetic counseling and sharing the news with my family. Thankfully, my kids were receptive and eager to learn if they were CDH1 positive. We proceeded with the testing. My sister, who also tested, learned that she was negative. That was good news. However, both of my children came back positive.
Suddenly, my kids were on this gastric cancer journey with me. They met with genetic counselors, consulted with Dr. Woo, and began evaluating their options. With such high odds that both of them would develop cancer at some point, it was necessary to begin testing and planning now. My daughter faced a double whammy with high gastric cancer diagnosis odds as well as increased risk for lobular breast cancer.
Both of my children decided to do whatever was needed to avoid getting this awful disease. For Tyler, that meant getting a total gastrectomy in his mid-20s. For Kori, she’d receive a total gastrectomy as well as a double mastectomy, all before age 30.
Greg’s Total Gastrectomy
The week before Thanksgiving, I visited with Dr. Woo. First, she did a small workup to see how I was looking. During the process, she casually asked when my surgery was scheduled for. Surprised, I told her that I thought I’d be receiving that news from her today. She was alarmed to discover that I hadn’t been scheduled yet.
Immediately, she picked up the phone and made a flurry of calls. Unfortunately, it wasn’t possible to get me in for surgery immediately, so I would have to wait until December 27th. This also meant that I’d need to have additional FLOT treatments beforehand to keep the cancer at bay.
The end of December 2021 was a high-stakes time for our family. In addition to my total gastrectomy, both of the children were having biopsies done at City of Hope in Duarte.
The Day of the Surgery
After much anticipation, I went in for my total gastrectomy. The surgeon informed me that the surgery would take 6.5 hours. At 7:30 that morning, I was put under anesthesia for the procedure.
When I woke up, I recall being confused because the clock showed it was only 9:30 AM. I wondered if there had been some sort of issue that prevented the surgery. From what I’d read, surgeons will end the procedure if they discover that the cancer has spread beyond the stomach. Could this be the reason that my surgery ended so quickly?
Kristie reassured me via text that the surgery was complete – it turns out that I had been on the operating table for 18 hours! It was 9:30 AM, but not on the same day. My esophagus was weak following the FLOT treatments, and it took the operating team multiple attempts to connect my esophagus to my intestine. Eventually, they had to go in above my diaphragm. They even had a thoracic specialist deflate my lung so that they could complete the process. I was thankful for the incredibly talented team that took care of me during such an arduous procedure.
Taking Time to Recover
Following the surgery, I began a lengthy recovery process. I was in the hospital for 11 days and down at home after that for practically three months. My diet was severely restricted at first. I received nutrients via an IV. Then, after lots of testing to ensure that the surgery was a success, I moved on to liquids and soft foods.
The total gastrectomy altered my eating habits. Even now, I chew my food more thoroughly than before. I eat smaller meals and consume food more frequently throughout the day.
Personally, I found the psychological element of recovery much more challenging than the physical element. I developed extreme food aversions, lost over 100 pounds, and underwent all sorts of strange bodily changes. Further, I still had two FLOT treatments left, and these were miserable. I spent nights dry heaving in the bathroom, unable to keep liquids or food down. It was a challenging time, and I relied heavily on Kristie to keep me going.
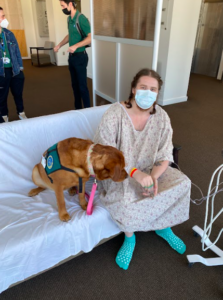 Tyler’s Gastric Cancer Diagnosis Story
Tyler’s Gastric Cancer Diagnosis Story
You’ll recall that Kori and Tyler were due to have their biopsies at the end of December as well. After extensive testing, we learned that Kori was currently cancer-free. This was great news. However, we also found out that Tyler already had stage 1 cancer at age 25.
Both of the kids already had their major procedures scheduled. My son had a particularly rough time with the total gastrectomy. He had an esophageal leak, which led to doctors placing a stent. But the stent migrated to his intestine and he had to have another emergency surgery to remove it. He spent two weeks in the hospital after the surgery and lost an extreme amount of weight.
Later, two weeks before his wedding in March, Tyler began having problems with swallowing. He texted Dr. Woo for help, and she immediately got him in for esophageal dilation. It turns out that the opening in his esophagus had shrunk to the size of the tip of a ballpoint pen.
Since the procedure, Tyler has endured multiple hospital stays, various dilations, and other complications. But he is cancer free, and for that, we’re extremely grateful.
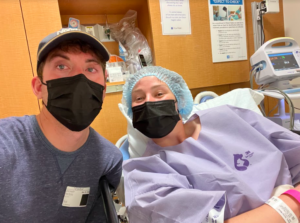 Kori’s Story
Kori’s Story
Kori, on the other hand, had a smooth stomach removal surgery and recovered the best out of all of us. Her double mastectomy went smoothly as well. Now, she is awaiting a breast reconstruction surgery which will take place later this year. This will be her last major procedure following the positive CDH1 test.
Q: You and your family have undoubtedly been through a lot since your stomach cancer diagnosis. What is your hope?
A: It has been a wild ride. We are grateful for the providers and caregivers who have helped us along the way, and we’re thankful for the genetic testing that revealed the CDH-1 mutation. We are also grateful to Dr. Woo for her incredible work.
Cancer is a life changer, but not a life ender. Our hope is to continually accomplish amazing things as a family and to inspire others to do the same. We aim to climb Mt. Whitney together next summer with our kids and other survivors to show that a gastric cancer diagnosis doesn’t have to stop you.
2023 Updates
In February of this year, I had a CT scan. The scan revealed a suspicious spot in one of the quadrants of my peritoneum, and the doctor recommended we look at it more closely. So, I had a follow-up with my surgeon, and she recommended a PET scan along with a diagnostic laparoscopy. She took biopsies of the concerning spots.
Unfortunately, the spots came back positive for cancer – which meant I officially had a stage 4 diagnosis. My doctor proposed a treatment plan that involved HIPEC, a process where heated chemotherapy is applied directly to the concerning spots. We’d do three rounds of HIPEC roughly six weeks apart. In between, I’d have FOLFOX chemotherapy and Opdivo.
The first two HIPEC treatments were quite difficult. Further, it was tricky to complete chemotherapy in between due to my low platelet count. Surprisingly, the later rounds of HIPEC were easier to manage.
In December, I’ll have another diagnostic laparoscopy, and we’ll decide if I need further HIPEC treatments from there. My last biopsies actually came back negative for cancer, so my doctor has tentatively declared NED. However, she emphasized that we’re in uncharted territory – cancer likes to hide in scar tissue, and we have to be vigilant about watching for it. At the same time, we don’t want to do more HIPEC procedures than necessary since HIPEC creates a lot of scar tissue. It’s a delicate balance.
This year has been full of ups and downs. At first, I thought this could be the beginning of the end. But the HIPECs have been effective so far, and I’m busy doing the things I love, like fishing and riding dirt bikes.
My kids are also doing wonderfully. Tyler had a revision surgery in April, and that proved to be an excellent choice. He’d struggled badly up to that point, but he’s finally putting on weight again and feeling much better. Kori medically retired from the Air Force this summer, and now she’s deciding what she’d like to do next. We are all living happily despite this rough road we’ve traveled together.

